
I recently spoke with Farrah Mateen, MD, PhD, of Massachusetts General Hospital and Harvard Medical School about the Bhutan Epilepsy Project. Dr. Mateen and her team are working on a unique project investigating the use of mobile EEG to diagnose seizure disorders in remote and under-resourced areas.
Bhutan Epilepsy Project
JESSICA KEENAN SMITH: Dr. Mateen, thank you for taking time out of your busy schedule to speak with Living Well With Epilepsy about the Bhutan Epilepsy Project. Would you start by describing this initiative?
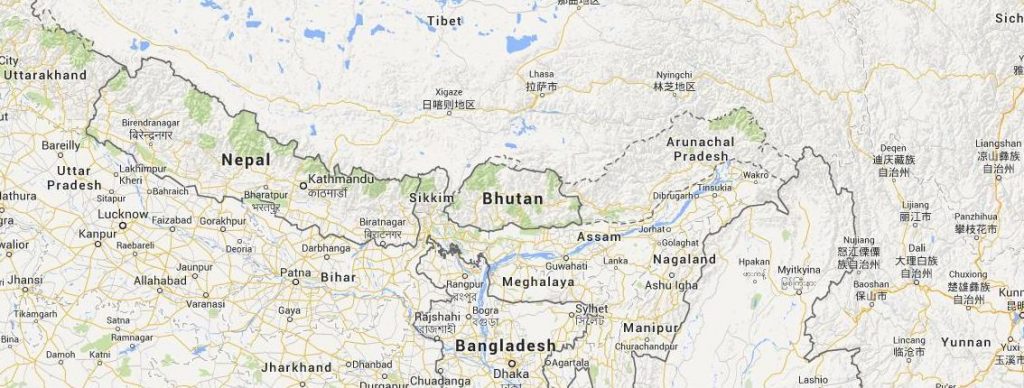
DR. FARRAH MATEEN: The Bhutan Epilepsy Project is a research endeavor to help improve the diagnosis of seizure disorders in Bhutan. It is aimed to improve the lives of people with seizures and suspected seizures in the Kingdom of Bhutan, a landlocked Himalayan country with a potentially high epilepsy burden. The project involves patients, neurologists, psychiatrists, traditional medicine practitioners, computer software engineers, EEG technicians, social scientists, and business planners and research coordinators.
SMITH: I have to be honest, I don’t know much about Bhutan. Can you describe the need for epilepsy diagnostics in the Kingdom of Bhutan?
MATEEN: The number of people living with epilepsy in Bhutan has not been formally studied epidemiologically, but up to 1 percent of the population may have epilepsy. That equates to approximately 10,000 people in the country. Epilepsy is often first diagnosed in children and we are aiming to enroll neonates (newborns) and children especially.
There is no neurologist in Bhutan. The care of people with epilepsy is handled by psychiatrists, including our project collaborator Dr. Damber Nirola.
EEG Technology Goes Mobile
 SMITH: How are you and your team implementing this study?
SMITH: How are you and your team implementing this study?
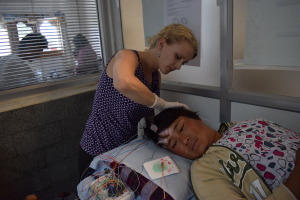
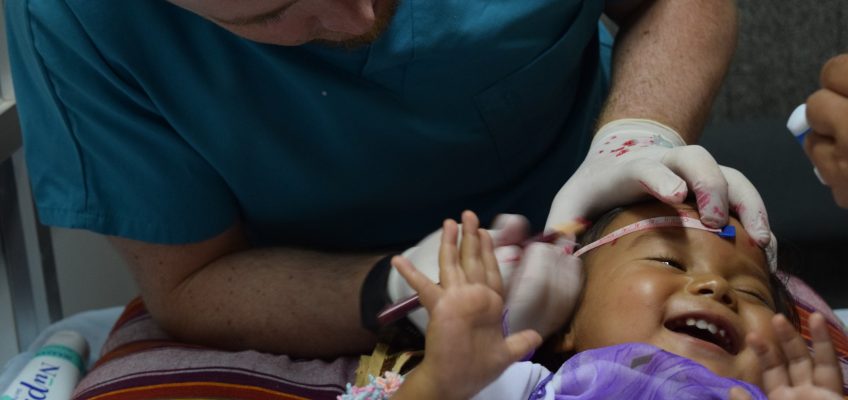
MATEEN: It is a clinical cohort study in which all participants are offered an opportunity to have a stationary EEG, smartphone EEG, brain MRI, and neurocysticercosis testing. It is an international collaborative project which uses software developed by the Danish Technical University’s lab (Principal Investigator Lab: Lars Kai Hansen, Dept of Applied Mathematics and Computer Science) for an EEG smartphone device. The project takes place primarily in the Jigme Dorji Wangchuk National Referral Hospital in Thimphu.
SMITH: Why is Bhutan the ideal site for this project?
MATEEN: They have a high uptake of new technologies including cell phones. Their uptake of mobile phones has been rapid and widespread, approximately the prevalence of cell phone usage in countries such as Canada! They also have a presumed high burden of epilepsy, likely due to the prevalence of preterm birth, genetics, and neurocysticercosis. Moreover, the geographic barriers to reaching the main referral center make the use of community-health level portable technologies ideal for the population.
Making a Difference
SMITH: How many patients are expected to benefit from this project?
MATEEN: We are exceeding our planned enrollment. So far, more than 100 people are recruited including more than 50% of people under age 18 years old. We hope to enroll 125 additional participants throughout November and potentially more people in early 2015.
SMITH: What is your involvement? How did you come to participate?
MATEEN: I am the principal investigator and developed the grant proposals. Through conversations with my collaborators, Dr. Damber Nirola, and before him, Dr. Chencho Dorji, both Bhutanese psychiatrists, I developed the project. I have been to Bhutan four times to operationalize the project so far.
SMITH: I’m curious how you have been able to roll out this study. Does the project have financial support?
MATEEN: We are thankful for the support of Grand Challenges Canada, funded by the Government of Canada, and the Thrasher Research Foundation (Early Career Award). Academically, the University of Ottawa, JDW National Referral Hospital, Danish Technical University, and Massachusetts General Hospital are all collaborators.
Removing Barriers to Care
 SMITH: What would success from this project look like to you?
SMITH: What would success from this project look like to you?
MATEEN: We hope the smartphone EEG will help diagnose seizures in this population and show value in a resource-limited setting. More importantly, we are pleased that people in Bhutan will access diagnostic care for seizures that may help direct their care.
I hope the project brings attention to the lives of people with epilepsy in resource-limited settings, explores and addresses their feelings of stigma, removes barriers to care, and optimizes their quality of life.
Most importantly, I have gained lifelong friendships with wonderful collaborators in Bhutan, Denmark, and beyond. I am very thankful to my research coordinators in Bhutan, Ms. Sonam Deki and Mr. Lhab Tshering. They are very inspiring in their dedication to the project, as are our participants who often come from many hours away to participate. In this sense, the project has already succeeded in my books.
SMITH: Dr. Mateen, thank you again for taking the time, especially since you are about to head off to Bhutan for another extended visit. I look forward to hearing more as this project continues.

Leave a Reply